
Quick answer: Success in obesity care is not measured by weight loss alone. A more complete picture includes metabolic health, cardiovascular health, quality of life, and long-term sustainability. Weight loss can be important, but markers like A1C can help show whether health is improving beyond the scale, especially for people with diabetes, prediabetes, or risk factors for type 2 diabetes.
When people think about obesity care, the scale is often the first thing they focus on. Weight loss is visible, easy to measure, and commonly used as a sign of progress.
But weight loss is only part of the story.
True progress in obesity care is not just about seeing a lower number on the scale. It can also be seen in A1C, blood pressure, cholesterol, energy levels, sleep quality, improved mobility, and healthier habits that last.
In the United States, obesity remains highly common. According to the CDC’s National Center for Health Statistics, the prevalence of obesity among U.S. adults was 40.3% during August 2021–August 2023. That means obesity care is not a niche health issue; it is relevant to the long-term health of millions of people. (CDC)
Key Takeaways
- Weight loss is an important part of obesity care, but it is not the only measure of success.
- A more complete obesity care plan may consider weight, metabolic health markers such as A1C, blood pressure, cholesterol, and triglycerides, along with energy, sleep, mobility, and long-term sustainability.
- A1C may be especially relevant for people with diabetes, prediabetes, or risk factors for type 2 diabetes.
- A1C is reported as a percentage and reflects average blood glucose levels over the past 2 to 3 months.
- Weight loss and A1C do not always improve at the same pace.
The scale can be helpful, but it has limits.
The Scale Shows Change, But Not the Whole Change
The Same Weight Loss Can Lead to Different Health Outcomes
Obesity Care Is About Health, Not Just Body Size
What Success in Obesity Care Should Really Include
Weight Change
Metabolic Health Improvement
Blood glucose is the amount of sugar circulating in the blood. When it remains high over time, it may signal insulin resistance and increased risk of type 2 diabetes and other health complications.
A1C, also known as hemoglobin A1c, reflects average blood sugar levels over the past 2–3 months. Higher A1C levels are associated with greater long-term exposure to elevated glucose and a higher risk of diabetes-related complications such as eye, kidney, and nerve damage.
Cardiovascular Health Markers
Energy, Sleep, and Quality of Life
Long-Term Sustainability
Success is not just early weight loss. It also means building habits and care plans that can be maintained over time.
In other words, obesity care is not just about asking, “How much weight did I lose?” It is also about asking, “What’s improving beyond my weight?”
Health Markers to Consider Beyond Weight

| What to Track | Why It Matters in Obesity Care |
|---|---|
| Weight | Shows body weight change over time |
| Waist circumference | Helps assess abdominal obesity and related risk |
| A1C | Shows average blood sugar over the past 2 to 3 months |
| Blood sugar | Helps understand glucose patterns and metabolic health |
| Blood pressure | Helps assess cardiovascular risk |
| Cholesterol | Helps evaluate heart and metabolic risk |
| Triglycerides | Can reflect metabolic and cardiovascular risk |
| Energy and sleep | Reflect day-to-day quality of life |
| Physical function | Shows whether daily movement and mobility are improving |
Not every person needs to track every marker in the same way. The right approach depends on personal health history, risk factors, and guidance from a healthcare provider.
Still, the main point is simple: the scale is only one data point.
Why A1C Matters in Obesity Care
| Weight Status | Diabetes Prevalence (U.S. Adults) |
|---|---|
| Underweight or Normal Weight | 6.8% |
| Overweight | 12.3% |
| Obesity | 24.2% |
What A1C Measures
A1C is reported as a percentage and reflects average blood glucose levels over the past 2 to 3 months. A higher A1C percentage indicates higher average blood glucose during that period.
The CDC explains that A1C reflects the percentage of red blood cells with sugar-coated hemoglobin, which is why it gives a longer-term view of blood sugar rather than a single moment-in-time reading.
Because A1C reflects long-term glucose exposure, higher levels are associated with a greater risk of diabetes-related vascular complications such as eye, kidney, nerve, and cardiovascular disease.
In general, an A1C level below 5.7% is considered normal, 5.7% to 6.4% indicates prediabetes, and 6.5% or higher indicates diabetes. These ranges should be interpreted with a healthcare provider.
A1C Shows What the Scale Cannot
In obesity care, this can be useful because weight and blood sugar do not always change at the same pace.
A person may lose weight but still have A1C levels that remain higher than expected. Another person may see improvements in blood sugar habits before major changes show up on the scale.
This does not mean one marker is more important than the other. It means they are measuring different parts of the health picture.
A1C Helps Provide a Longer-Term View of Blood Glucose Control
Daily glucose data can show short-term patterns, while A1C provides a longer-term view of blood glucose control. (Learn More) In obesity care, this longer-term view can help patients and healthcare providers better understand whether metabolic health is improving beyond changes in body weight.
Why Weight Loss and A1C May Not Always Move Together
Weight loss and A1C are connected, but they are not the same measurement. Weight reflects body mass at a point in time, while A1C reflects average blood glucose over the past 2 to 3 months.
It is natural to expect that if weight goes down, blood glucose markers will automatically improve. Often, weight loss can support better metabolic health. But the relationship is not always immediate or perfectly linear. As the graph below illustrates, people can experience very different patterns over time. In some cases, weight may improve before A1C changes. In others, A1C may improve even when weight loss is modest.
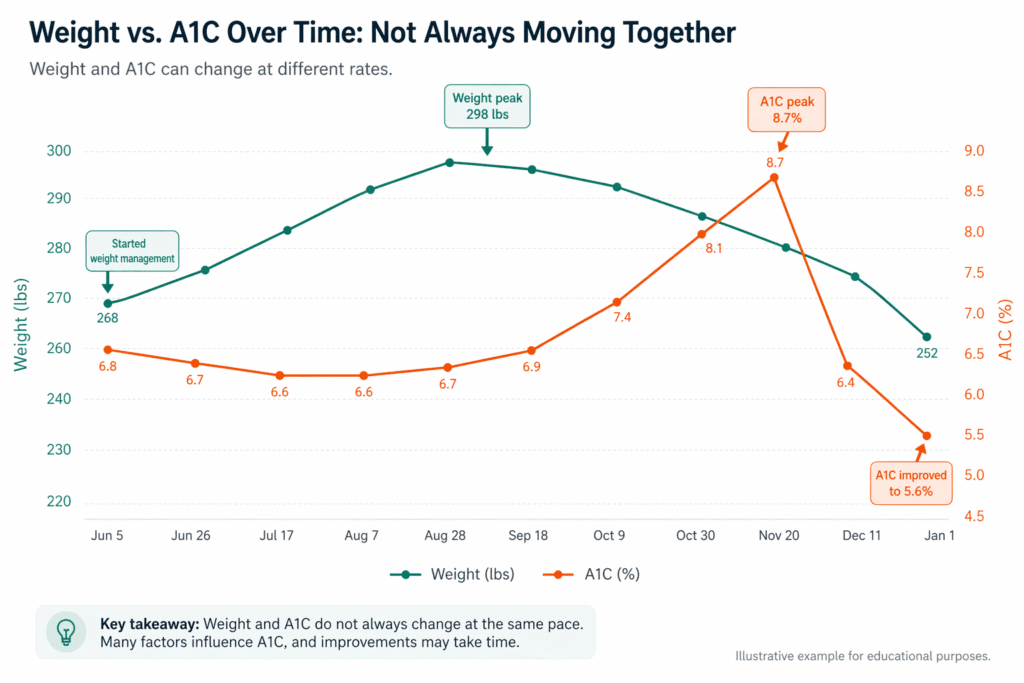
Several factors may affect A1C during obesity care, including:
- How long blood sugar has been elevated
- Changes in eating patterns
- Physical activity
- Sleep and stress
- Medication use
- Insulin resistance
- Individual biology
That is why a person may ask, “Why am I losing weight but my A1C is still high?”
The answer may be different for each person, and it is a good question to discuss with a healthcare provider.
The important point is that weight loss and A1C are connected, but they are not the same measurement.
How Can You Tell If Your Health Is Improving Beyond the Scale?
Progress in obesity care can show up in many ways.
Some people may notice they have more energy. Others may sleep better, feel more consistent with meals, move more easily, or see improvements in lab results. Some may find that their blood sugar patterns become more stable. Others may see improvements in blood pressure, cholesterol, or triglycerides.
These changes matter because obesity care is not only about short-term weight loss. It is about long-term health.
A more complete view of progress may include questions like:
- Is my energy improving?
- Are my eating patterns more consistent?
- Are my blood sugar markers improving?
- Are my lab values moving in the right direction?
- Can I maintain these changes over time?
- Do I understand my personal health risks better than before?
This kind of broader view can help people avoid judging success by the scale alone.
Questions to Ask Your Healthcare Provider
If you are receiving obesity care or working on weight loss, it may be helpful to ask your healthcare provider how to measure progress beyond weight.
Questions may include:
- What should I track besides body weight?
- Should I monitor blood sugar or A1C?
- How often should I check metabolic health markers?
- What health markers matter most for my personal risk profile?
- How should I define success in my obesity care plan?
- If my weight is changing but my A1C is not, what should I do next?
- Do I have risk factors for prediabetes or type 2 diabetes?
These conversations can help make obesity care more personalized and more focused on long-term health outcomes.
The Bottom Line: Obesity Care Is About More Than Weight Loss
Weight loss can be an important part of obesity care, but it is not the whole story.
A more complete view of success includes metabolic health, cardiovascular risk, daily quality of life, and long-term sustainability.
A1C is one marker that can help show what is happening beyond the scale, especially for people with diabetes, prediabetes, or risk factors for type 2 diabetes.
The scale can tell you that your weight is changing. Markers like A1C can help tell a deeper story about your metabolic health.
Frequently Asked Questions (FAQ)
Does Weight Loss Always Improve A1C?
No, weight loss does not always improve A1C immediately.
Weight loss can support better metabolic health, but A1C and body weight do not always change at the same pace. Because A1C reflects average blood glucose over the past 2 to 3 months, changes in body weight are not always immediately reflected in A1C results. Results can also depend on factors such as eating patterns, physical activity, medication use, insulin resistance, and starting blood sugar levels.
Why Is My A1C Still High Even Though I Am Losing Weight?
A1C may remain high during weight loss because blood sugar changes can take time and depend on several factors. These may include insulin resistance, diet changes that are still in progress, medication factors, sleep, stress, or how long blood sugar has been elevated.
A healthcare provider can help interpret your A1C in the context of your full health picture.
What Health Markers Matter Besides Body Weight in Obesity Care?
Health markers besides body weight may include A1C, blood sugar, blood pressure, cholesterol, triglycerides, waist circumference, sleep, energy, and physical function. The right markers to track depend on personal health history and treatment goals.
Is A1C Only for People With Diabetes?
No, A1C is not only relevant after a diabetes diagnosis. A1C is commonly used to diagnose and monitor diabetes and prediabetes, but it can also be part of a broader conversation about metabolic health for people who have risk factors. Healthcare professionals use A1C, sometimes with other tests, to help diagnose type 2 diabetes and prediabetes. (NIH)
For people with obesity, prediabetes, diabetes, or other risk factors for type 2 diabetes, A1C may be worth discussing with a healthcare provider.
How Do You Measure Success in Obesity Care?
Success in obesity care can include weight loss, but it should also include improvements in metabolic health, quality of life, cardiovascular risk factors, and long-term sustainability. A more complete care plan looks beyond the scale.
According to CDC data, diabetes prevalence was 24.2% among adults with obesity. If you have obesity and any of the following risk factors:
- Elevated blood sugar
- Family history of diabetes
- Physical inactivity
- History of gestational diabetes







